Diabetes mellitus, commonly referred to as diabetes, is a metabolic disorder that results in constantly elevated blood glucose levels (hyperglycaemia). Our blood glucose levels are usually regulated by insulin, a hormone secreted by the pancreas in response to elevated blood glucose levels.
Insulin facilitates the absorption of excess glucose in blood circulation into liver, fat and skeletal muscle cells, where it gets converted to glycogen or fat, accordingly. When blood glucose levels are low, insulin secretion is inhibited and glycogen and/or fat molecules are broken down into glucose and re-released into circulation as required.
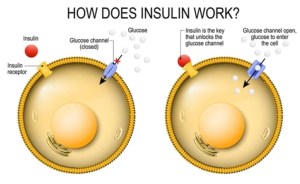
Image from News Medical
In Type 1 (insulin-dependent) diabetes, blood glucose levels rise as a result of the body destroying insulin producing-beta cells in the pancreas’ islets of Langerhans in an autoimmune response, thereby disrupting insulin production. In Type 2 (non-insulin-dependent) diabetes, either the beta cells produce insufficient insulin, or the body is unable to effectively use the insulin produced to regulate blood glucose levels. The latter phenomenon is referred to as insulin resistance.
The global prevalence of diabetes was estimated to be nearly 9.5% as at 2019, with the figure showing an increasingly upward trend over the past few decades. Of this, around 10% of cases are Type 1 and around 90% of cases are Type 2. According to the WHO, diabetes-related complications are one of the leading causes of death globally.
Symptoms
The symptoms for diabetes are more or less common for both Type 1 and Type 2. These include:
- frequent urination
- increased thirst and hunger
- unintended weight loss
- fatigue
- slow healing of wounds or sores
- blurry vision
- numbness or tingling in hands or feet
- more frequent infections (such as thrush)
- dry skin
In addition, diabetic patients may feel irritable at times, and those with Type 2 diabetes in particular may experience pigmentation in some areas of their body, such as around the neck and armpits.
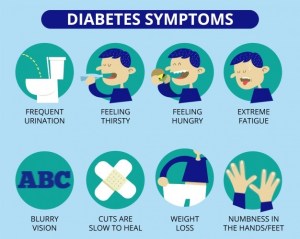
Image from Freepik
Complications
The long-term presence of excess glucose in blood can be damaging to blood vessels, leading to potential complications in several of the body’s vital organs. These may include:
- cardiovascular disease, such as angina (chest pain), atherosclerosis (narrowing of arteries), cardiac arrest (heart attack), stroke, high blood pressure
- renal disease, where damage to capillaries involved in filtration can result in severe damage to the kidneys (nephropathy)
- neurological disease, where damage to capillaries that nourish nerves can result in damage to nerves (neuropathy) that begin at extremities and eventually may spread further into the body; damage to nerves in the gastrointestinal tract may cause nausea, vomiting, diarrhoea or constipation
- eye disease, such as impaired vision, cataract, glaucoma, damage to the retina (diabetic retinopathy) and even potential blindness
- skin and mouth diseases, as susceptibility to bacterial and fungal infections increases
- complications in pregnancy, such as an increased risk of miscarriage, stillbirth and birth defects, as well as ketoacidosis, preeclampsia, retinopathy and high blood pressure in the mother
- diabetic ketoacidosis (DKA), where the body starts breaking down fat for energy, potentially leading to a diabetic coma (usually with Type 1)
- hyperosmolar hyperglycaemic state (HHS), where the body gets severely dehydrated as it tries to get rid of excess sugar (usually with Type 2)
Causes
Type 1 diabetes is autoimmune in nature. This means that the body’s immune system inadvertently attacks its own cells (beta cells in the pancreas’ islets of Langerhans), thereby inhibiting their function – which is the synthesis and secretion of insulin. As a result, excess glucose does not get extracted from circulation, resulting in high blood glucose levels. The presence of certain genes may also increase the likelihood of developing Type 1 diabetes, with family history possibly playing a role in incidence.
Type 2 diabetes is a result of an insufficient production of insulin, or insulin resistance. Risk factors for this condition include:
- prevalence of prediabetes (where blood glucose levels are higher than usual, but not high enough to be classified as diabetes)
- obesity
- an inactive lifestyle
- family history of diabetes
- previous incidence of gestational diabetes (diabetes during pregnancy)
- certain ethnic backgrounds, such as Latin American, African-American, South Asian
Diagnosis
Symptoms of Type 1 diabetes may develop over a matter of weeks or months and are usually more severe than those of Type 2. They are therefore mostly detected at an early age – often in childhood itself, although people up to the age of 40 years may be diagnosed with Type 1 diabetes. Symptoms of Type 2 diabetes usually develop over several years and may not be very obvious at first. These cases may therefore initially go undetected, or be mistaken for other conditions. Type 2 diabetes is often diagnosed in adults, sometimes later on in life.
Usually, a simple blood test is sufficient to determine blood glucose levels. Ideally, this would be a fasting blood sugar (FBS) test, where the blood sample is drawn after 8-10 hours of fasting. In certain cases where a quick result is required, a random blood sugar (RBS) test may be carried out without fasting.
According to the guidelines given by NHS-affiliated ‘Diabetes My Way’:
- for non-diabetic individuals, normal blood glucose levels should range from 3.5 – 5.5 mmol/L (63 – 99 mg/dL) before meals, and < 8.0 mmol/L (< 144 mg/dL) two hours after meals
- for diabetic individuals, the target figures in Table 1 are recommended
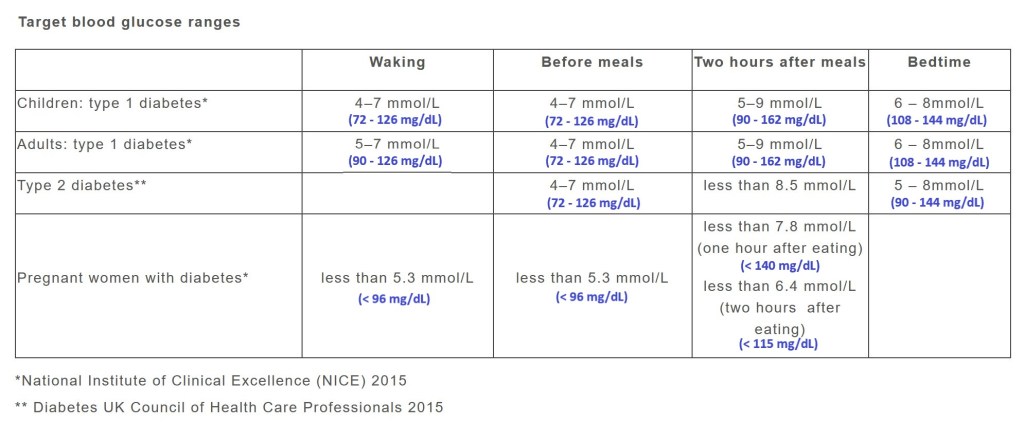
Your doctor may also recommend doing an HbA1c (haemoglobin A1c) test which estimates your blood glucose levels over the past three months – particularly if you do not regularly monitor blood sugar levels at home. This works on the basis that haemoglobin-carrying red blood cells usually last for around 8-12 weeks. Following are the target figures published on ‘Diabetes My Way’:
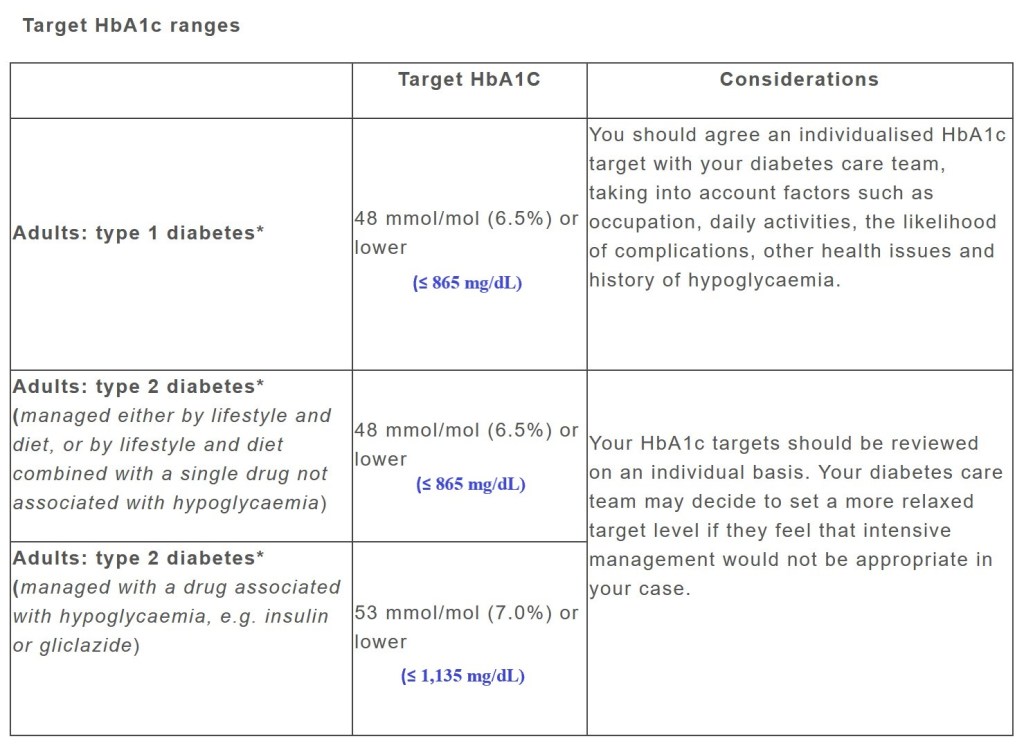
If Type 1 diabetes is suspected, an additional blood test to check for autoantibodies as well as a urine test to check for ketones may also be prescribed.
It is important to monitor blood glucose levels regularly if you have been diagnosed with diabetes, so that treatment could be adjusted accordingly. A DIY finger-prick home kit may be used for daily or frequent monitoring in cases of:
- Type 1 diabetes
- Type 2 diabetes being treated with insulin (or other injectable substitutes)
- women with gestational diabetes (diabetes that becomes prevalent during pregnancy)
However, in cases where Type 2 diabetes is being controlled by changes in diet and lifestyle or with oral medication, carrying out an HbA1c test every 6 months or so would suffice – unless any changes or complications are observed.
Prevention
There is no means of preventing Type 1 diabetes since it is a condition related to an autoimmune reaction, generally with a genetic predisposition.
However, certain measures may help to prevent or delay the onset of Type 2 diabetes, particularly if there is a known risk of the condition. These include:
- maintaining a healthy diet that includes plenty of fruit and vegetable
- avoiding frequent intake of sugary foods and beverages
- moderating intake of carbohydrates (as these break down into sugars)
- drinking plenty of water
- maintaining an active lifestyle and engaging in some regular form of exercise
- maintaining a healthy body weight and working to shed any extra weight
- providing constant parental guidance to children, in terms of incorporating fruits and vegetables into their diet, minimising sugary food and drink, encouraging some sort of daily physical activity, serving small portions of food
Treatment
While there is no cure for diabetes, certain measures may be taken in order to maintain a controlled and healthy blood glucose level.
In the case of Type 1 diabetes, intake of insulin is inevitable as the insulin-secreting cells themselves are destroyed. This is most commonly done in the form of injections (often self-administered). In certain serious cases, a doctor may suggest the use of a more complex insulin ‘pump’, which is an electronic device with a cannula, that maintains the body’s insulin levels day and night. It is important to simultaneously maintain a healthy diet (low in sugars and carbs) and an active lifestyle.
In the event where insulin is taken on a regular basis, caution should be taken to monitor blood glucose levels frequently in order to ensure that the dosage taken would not lead to hypoglycaemia (low blood sugar). If a patient repeatedly experiences ‘hypo’ attacks, islet cell transplantation may be recommended, if suitable.
In the case of Type 2 diabetes, insulin may or may not be required – your doctor would have to determine this. In some (early or mild) cases, switching to a healthy diet and incorporating exercise into your daily routine (both of which would support weight loss) alone might help to put the diabetes into remission. However, in other cases, the first line of treatment is typically a suitable dose of metformin along with the said lifestyle changes. Other medication such as sulphonylureas (to stimulate insulin production from the pancreas) or tablets to aid weight loss may also be prescribed.
Cover illustration from Wonderwall.sg

all your articles are super informative. keep continuing.
LikeLike
Thank you! 🙂
LikeLike