Polycystic ovarian syndrome, or PCOS as it is commonly known, is a condition that affects around one in ten women around the world. It is caused by a hormonal imbalance which can bring about several metabolic and physical changes in the sufferer.
The ovaries (left and right) are the organs in the female reproductive system which are responsible for the formation, maturation and release of an ovum (egg) every month. The egg begins development as a follicle, eventually growing into a mature ovum which gets released for fertilisation at ovulation. If fertilisation occurs, the ovum develops into a zygote and then an embryo which gets embedded in the uterus. If fertilisation does not occur, the ovum disintegrates and what is left of it (the corpus luteum) is expelled prior to the onset of the next cycle.
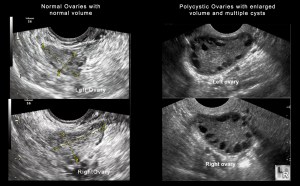
Usually, a single ovum is formed during one cycle. However, in the case of PCOS, several follicles mature and remain in the ovaries at a given time, giving rise to the observation of a ‘polycystic’ appearance of the ovaries in ultrasound scans. This condition may give rise to anovulatory or irregular cycles.

Image from Mayo Clinic
Symptoms
PCOS may be asymptomatic in some cases, and therefore may go unnoticed for long periods of time. In cases where symptoms are present, observation may occur as early as at menarche (when a girl starts menstruating) or later on in their life (20’s or 30’s). Symptoms that may usually be observed include:
- irregular or absent menstrual cycle
- hirsutism (excessive hair growth on the face, abdomen and legs)
- acne (on the face, back, chest)
- weight gain (particularly around the waist and hips)
- hair thinning and/or male balding pattern
Causes
Although it is not entirely clear as to what the exact cause of PCOS is, it is widely believed that the disease is hereditary in nature. Hence, women with a family history of PCOS, or even a family history of Type 2 diabetes, are at a greater risk of developing PCOS.
Insulin resistance and being overweight are also believed to be risk factors for PCOS as both scenarios increase the level of unused or ‘lazy’ insulin in the body. An increased amount of insulin leads to an increased level of androgens, or male hormones, (mostly testosterone) in the body. This subsequently leads to the incidence of some or all of the symptoms discussed above.
Complications
There are certain complications that could arise in the long run for individuals affected by PCOS. These include:
- an increased risk of Type 2 diabetes due to insulin resistance
- an increased risk of cardiac disease and high blood pressure
- an increased risk of endometrial cancer as insulin resistance, irregular ovulation and weight gain could cause thickening of the endometrium (uterine lining)
- fertility issues due to anovulation or irregular ovulation (PCOS is the main cause of infertility among women which, however, is often treatable)
- low self-esteem as a result of some of the symptoms observed
- depression and anxiety
Prevention
If you have a known family history of PCOS or Type 2 diabetes, a few recommended practices to lower your risk of PCOS are:
- leading an active lifestyle
- maintaining a predominantly organic diet
- avoiding processed and genetically modified (GM) foods
- controlling your intake of sugar-rich foods
However, understandably, there is no guarantee that these practices would nullify the odds of you developing the disease.
Diagnosis
Observation of two or more of the symptoms discussed is a strong indication that an individual might be suffering from PCOS. This can be confirmed using:
- a blood test to check for insulin resistance – measure insulin and blood glucose levels at 0 hrs, 1 hr and 2 hrs post-consumption of a dose of glucose
- a blood test to check levels of reproductive hormones oestrogen, progesterone, follicle stimulating hormone (FSH), leutenizing hormone (LH) and testosterone – this is usually done around the third or fourth day of the menstrual cycle
- an ultrasound scan to observe the presence of multiple follicles, which appear as cysts, in slightly enlarged ovaries
Treatment
There is no known permanent treatment for PCOS, and most treatment paths tackle symptoms rather than the underlying cause. The most common form of treatment administered by gynaecologists for women who do not want to get pregnant is the contraceptive pill. However, this mostly only helps to regulate an irregular cycle, and may help to reduce hirsutism and acne. Moreover, the safety of long-term use of the contraceptive pill is still a topic of debate.
In order to deal with the disease at the grassroots level, it is important to address the issue of insulin resistance. Metformin (sold as Glucophage), which is used in the treatment of Type 2 diabetes, has been known to improve the body’s use of insulin, making its action more efficient and thereby regulating the level of the hormone in the body. This, in turn, can help to regulate levels of androgens in the body. As a result, symptoms caused by increased levels of insulin and androgens may be alleviated or better controlled. If the patient is overweight, it would be greatly beneficial to get into a regular workout pattern and shed a few (usually stubborn) kilos. There are no known complications related to the long-term use of metformin.
Spironolactone (sold as Aldactone) is another drug which can help reduce the binding of androgens to receptors within the body, hence helping to ease symptoms such as hair loss, hirsutism and acne.
In combination with the above drugs, myo-inositol is a supplement of the vitamin B family that is known to help improve ovarian function, and subsequently to deal with cycle irregularity and fertility issues, by playing a role in regulating the hormones FSH and insulin.
Treatment to control physical symptoms may also be sought concurrently. A topical solution or ointment may be used to control acne. Bear in mind that given the hormonal nature of the cause, it can be rather challenging to control this type of acne. Hair removing agents or laser hair removal may be used to deal with hirsutism. Such measures may help the individual to feel better about themselves and boost their self-esteem, helping to keep anxiety and depression in check.
Cover illustration from Juniper Family Health.

2 Comments Add yours