In a strict sense, ‘chemotherapy’ refers to the use of chemical drugs to treat any given illness. However, it is most commonly and almost solely used with reference to the use of drugs in the treatment of cancer, which is what this article focuses on.
Contrary to surgery and radiation therapy, both of which target a specific site, chemotherapy (‘chemo’) is considered to be a more systemic form of treatment as it targets cancer cells around the body. Hence, it can help not only to destroy cancer cells at the origin (primary tumour), but can also target cancer cells that have spread (metastasised) to other parts of the body.
Mode of Action
Cancer cells generally grow and divide more rapidly than normal body cells, and it is this characteristic that is targeted by chemotherapy. This usually results from some sort of genetic mutation or damage in a cell’s DNA that results in uncontrolled cell division.
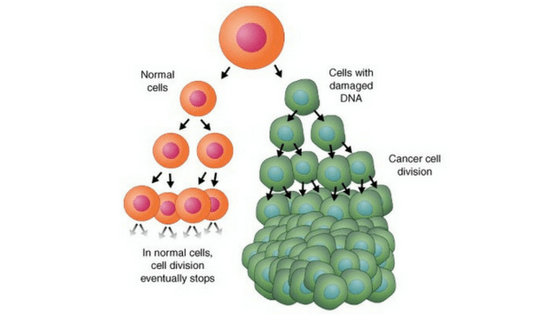
Illustration from Nutrition Can Heal
Chemotherapy drugs are effective against rapidly dividing cells, and therefore primarily target the rapidly dividing cancer cells once inside the body. Treatment may last from between weeks to months, and is usually administered in several rounds – depending on the nature and spread of the cancer.

Illustration from Health Direct
Intentions of Use
The intention with which chemotherapy is carried out may differ from patient to patient, depending on the type and size of tumour and degree of spread. It may therefore be used as:
- curative chemotherapy – for a complete cure of the cancer
- chemoradiation therapy – in conjunction with radiation therapy, to make the latter more effective
- neo–adjuvant chemotherapy – pre-surgery
- adjuvant chemotherapy – to prevent the recurrence of the cancer, post-surgery or post-radiation
- palliative chemotherapy – to alleviate symptoms where a cure is not possible
Modes of Administration
There are two main modes of administering chemotherapy to a patient:
- intravenous chemotherapy – This involves slowly releasing the drug directly into a vein via a cannula (tube temporarily placed into a vein in the lower arm), peripherally inserted central catheter (PICC) (tube inserted into the arm for a few weeks or months), central line (tube inserted into a vein near the heart through the chest), or an implanted port (inserted under the skin until course of treatment is completed). The patient ideally receives each dose of chemotherapy at the hospital.
- oral chemotherapy – This is usually given in the form of tablets which can be taken at home following a hospital check-up at the beginning of each round of treatment.
Less common forms of administration include subcutaneous (below the skin) injections, intramuscular (into a muscle) injections, intrathecal (into the spine) injections and skin creams.
Precautions
When having chemotherapy, it is best to speak to your oncologist about starting or continuing with any other medications as these may have adverse effects in combination.
It is also not advisable to become pregnant (whether it is the male or female partner receiving treatment) while undergoing chemotherapy as there is a significant likelihood of birth defects.
Side Effects
While the side effects of chemotherapy usually only last during and for a while after therapy, they can be intense in some cases, and may vary between patients. These mostly occur because, although the drugs are meant to target cancer cells, they may also affect other cells in our body that also multiply at a relatively higher rate than most other body cells, such as those that line our gut, skin and hair follicles.
Some of the most common side effects experienced include:
- fatigue and subsequent difficulty in carrying out everyday tasks – it may help to get plenty of rest, keep exercise to a minimum and avoid strenuous activities
- nausea or vomiting – it may help to take an anti-emetic prescribed by your doctor
- hair loss, mostly from the head but sometimes also from the face, arms and legs (regrowth usually commences once treatment stops, but hair may be straighter/curlier and a different shade than previous) – it may help to wear a cold cap during therapy so as to reduce the flow of blood containing drugs to the scalp
- loss of appetite – it may help to have a few smaller, healthier snacks during the day rather that three large meals, and to slowly sip water and drinks through a straw
- bleeding and bruising as therapy may lower platelet count – it may help to get medical advice on how to keep platelet levels up
- mouth sores, ulcers, dryness, bad breath, reduced sense of taste – it may help to avoid spicy, sharp or salty foods and to be gentle when brushing teeth and gargling
- anaemia as therapy may lower red blood cell (RBC) count – it may help to increase the iron content in your diet to avoid conditions such as iron deficiency anaemia
- diarrhoea or constipation – it may help to take suitable medication recommended by your doctor
- increased risk of infection as therapy may lower the body’s immunity – it may help to maintain a high level of personal hygiene, avoid close contact with outsiders (particularly if they are ill) and get the flu vaccine and any other relevant vaccines beforehand
- dry, sore, discoloured or sensitive skin – it may help to use a mild moisturiser and avoid direct exposure to the sun and extreme temperatures
- brittle or flaky nails – it may help to use a light moisturiser or moisturising nail varnish
- insomnia – it may help to maintain a regular sleep cycle, avoid stimulants before bedtime and avoid screen time before going to sleep
- reduced concentration and memory – it may help to do some mental exercises, maintain a healthy diet and rest well
- decreased libido – this usually returns to normal after cessation of treatment
- fertility issues, which may be temporary or permanent – it may help to speak to your doctor in advance and consider having eggs or sperm frozen beforehand
- emotional distress as a result of the pain of the treatment itself, but more often because of the challenging side effects that may accompany it – it is important to speak with family and friends or get professional help in order to support your mental health and well-being
Given the intense nature of side effects experienced by most recipients of chemotherapy, the decision on whether treatment should be administered or not sometimes comes down to a question of quality versus quantity. In the event where there appears to be no cure, one may ask if it is worth going through such side effects and compromising on quality of life for a short extension of it – particularly if the patient is already suffering as a result of the cancer. However, in cases where there is a more positive prognosis, chemotherapy is often administered without question in order to cure or support the cure of the cancer.
Cover illustration from iStock

One Comment Add yours