Vitiligo is a non-communicable, dermatological condition that affects about 0.5% – 1.0% of the world’s population. It is characterised by the appearance of pale/white coloured patches on the skin and is usually progressive in nature. The condition is more apparent in people with darker skin due to a greater contrast, however ethnicity is not a risk factor for the disease.
An individual’s skin and hair colour are determined by the presence of melanin, a pigmentation protein produced by specialised cells under the skin called melanocytes.
A lack of melanin due to insufficient working melanocytes is what causes some area(s) of the skin, and any hair above, to appear pale or white in colour. In some cases, the same phenomenon may occur on the scalp, causing patches of grey hair to appear.
These patches usually start off pale and small in size, getting lighter and gradually spreading over time, sometimes merging with patches originating at other parts of the body to become larger patches. The center of each patch is usually the whitest, while edges may appear smooth or jagged. Patches may appear slightly pink in colour where there are blood vessels underneath. There is no apparent difference in skin texture.
Symptoms
The white patches that appear due to vitiligo may be generalised or localised in nature. As such, categorisation may be done as follows:
- Generalised vitiligo (bilateral):
- > Non-segmental / vulgaris / common – patches appear to be symmetrical on both sides of the body and are commonly found on the back of one’s hands, arms, elbows, knees, feet and skin around openings such as the eyes; accounts for about 90% of cases
- > Acrofacial – patches are limited to face, head, hands and feet
- > Universal – patches cover around 80-90% of the skin; very rare
- Localised (unilateral):
- > Segmental – uni-, bi- or multi-segmental patches are present in only one part on one side of the body; more common among children
- > Focal – non-segmental isolated patches are found in one area on one side of the body
- > Mucosal – patches are found mostly around the mouth and other mucosal membranes
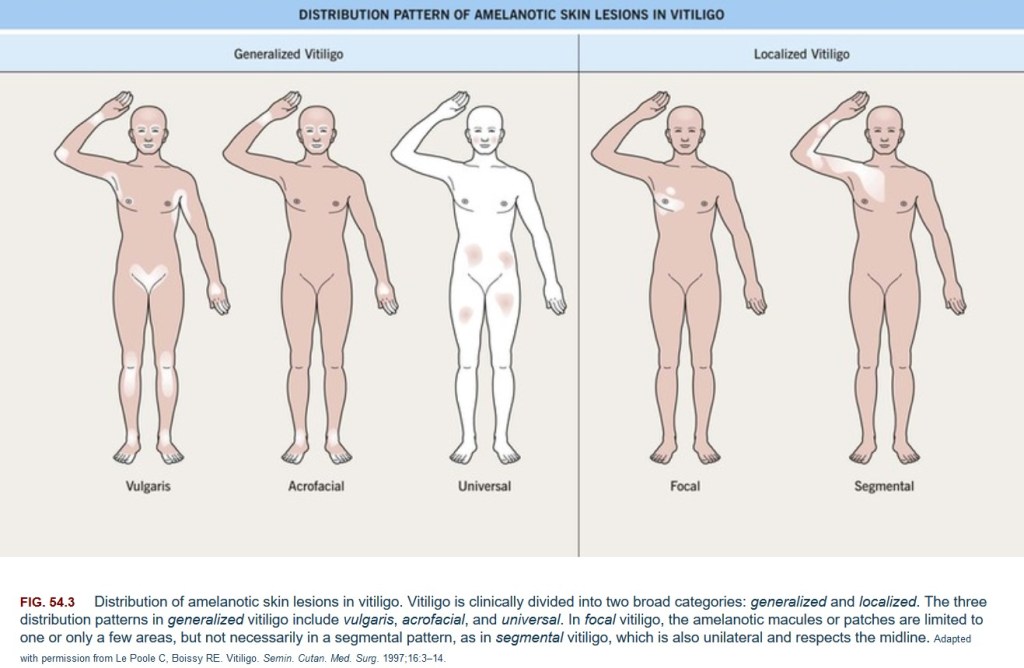
Image from clinicalgate.com
Causes
While the exact cause of vitiligo is not definitely established, it is largely believed that:
- generalised vitiligo is mainly caused by an autoimmune response. As such, the compromised immune system attacks the body’s own melanocytes, thereby decreasing the number of working cells that produce melanin pigment. Individuals with other autoimmune diseases, or with a family history of vitiligo or autoimmune disease are believed to be at greater risk of developing the disease.
- localised vitiligo is mainly caused by neurochemicals released by the skin’s nerve endings. These neurochemicals are toxic to and destroy melanocytes.
- both types may also be initiated by other trigger factors such as skin damage (e.g. cuts and burns), chemical exposure and stressful events.
Complications
While there is no particular discomfort experienced by vitiligo patients, there are a few, mostly mild, complications that might be associated with the condition:
- occasional itchiness
- increased sunburn where patches are present as the skin is more sensitive in these areas
- possible association with other autoimmune diseases such as hyperthyroidism
- possible association with ophthalmic inflammation and auditory issues
- low self-esteem and subsequent depression as a result of changed physical appearance
Prevention
There are no methods as such to prevent the incidence of either form of vitiligo.
The only thinkable piece of advice would be to protect one’s skin from stress, harmful chemicals and excessive exposure to sun if there is a known family history of vitiligo or autoimmune disease.
Vitiligo patients are usually advised to protect affected areas of skin from the sun in order to prevent irritation, dryness and discomfort due to photosensitivity.
Apart from that, in cases where vitiligo is already prevalent, it is important for both the patient and their associates to understand the nature of the disease so as to be able to gain and provide, respectively, support for the individual to boost their confidence and keep depression at bay.
Treatment
Vitiligo is a condition that is non-reversible. However, there are a few treatment options available for day-to-day use, or to try to reduce the area or spread of white patches. These include:
- topical camouflage creams, which can be applied on patches to match natural skin colour
- topical steroids, which sometimes help to reduce spread of patches in non-segmental vitiligo with less than 10% of the skin affected; however, there are many side-effects associated with the use of steroids (such as skin streaking, thinning, inflammation, etc.)
- phototherapy, where skin is exposed to ultraviolet A (UVA) or ultraviolet B (UVB) light; often it is administered as PUVA (psoralen to increase photosensitivity followed by UVA), however there are risks involved such as an increased probability of cancer with UVA exposure
- skin grafting, where skin is taken from an unaffected area and used to replace skin in a small affected area; alternatively, melanocytes may be removed from healthy skin and transplanted into vitiligo areas; complications such as scarring exist with both procedures
- depigmentation, where normal skin is bleached to match the colour of vitiligo skin when the condition has affected more than 50% of the skin; this too comes with complications such as excessive sensitivity of skin due to reduced protection from melanin
Non-topical treatment options are not regularly sought and are usually resorted to when the condition has had a negative impact on the patient’s quality of life.
Cover illustration by Dasha Horb.
