Leprosy (or Hansen’s Disease) is a communicable, infectious disease that has, over centuries, been associated with continued social stigma. In ancient times, it was believed to be some form of divine “punishment”, while in more recent history it was thought to cause “limbs to fall off” of affected individuals. In this article, we delve into the science behind leprosy and look at facts that may help to de-stigmatise and understand the reality of the disease beyond widespread myth.
According to the World Health Organisation (WHO), leprosy was globally eliminated (but not eradicated) as a public health problem in 2000 (with a prevalence record of <1 per 10,000 population). However, global incidence still surpasses 200,000 cases per year, with WHO’s recorded tally for 2019 being 202,037 cases. The majority of these cases arise in India, Bangladesh, Brazil, Myanmar and Indonesia, while prevalence is also high in certain African countries such as Nigeria and Mozambique.
Symptoms
Leprosy primarily affects the skin, peripheral nerves, mucous membranes of the upper respiratory tract and/or eyes. Depending on the area(s) affected, infection may result in symptoms such as:
- patches of skin with thickening, stiffness, discolouration
- skin nodules (growths)
- painless lumps on the face and/or earlobes
- painless ulcers on the soles
- loss of eyebrows and/or eyelashes
- numbness of skin in areas where sensory nerves are affected
- muscle weakness, mostly in hands and feet, where motor nerves are affected
- hair loss and dry skin (due to hindered sweating process) where autonomous nerves are affected
- enlarged nerves, mostly around the sides of neck, elbows and knees
- problems with vision
- stuffy nose and/or nosebleeds
- inflammation (redness, pain) around the affected area(s)
- pain or sensitivity in nerves of the affected area(s)
- burning sensation on skin in affected area(s)
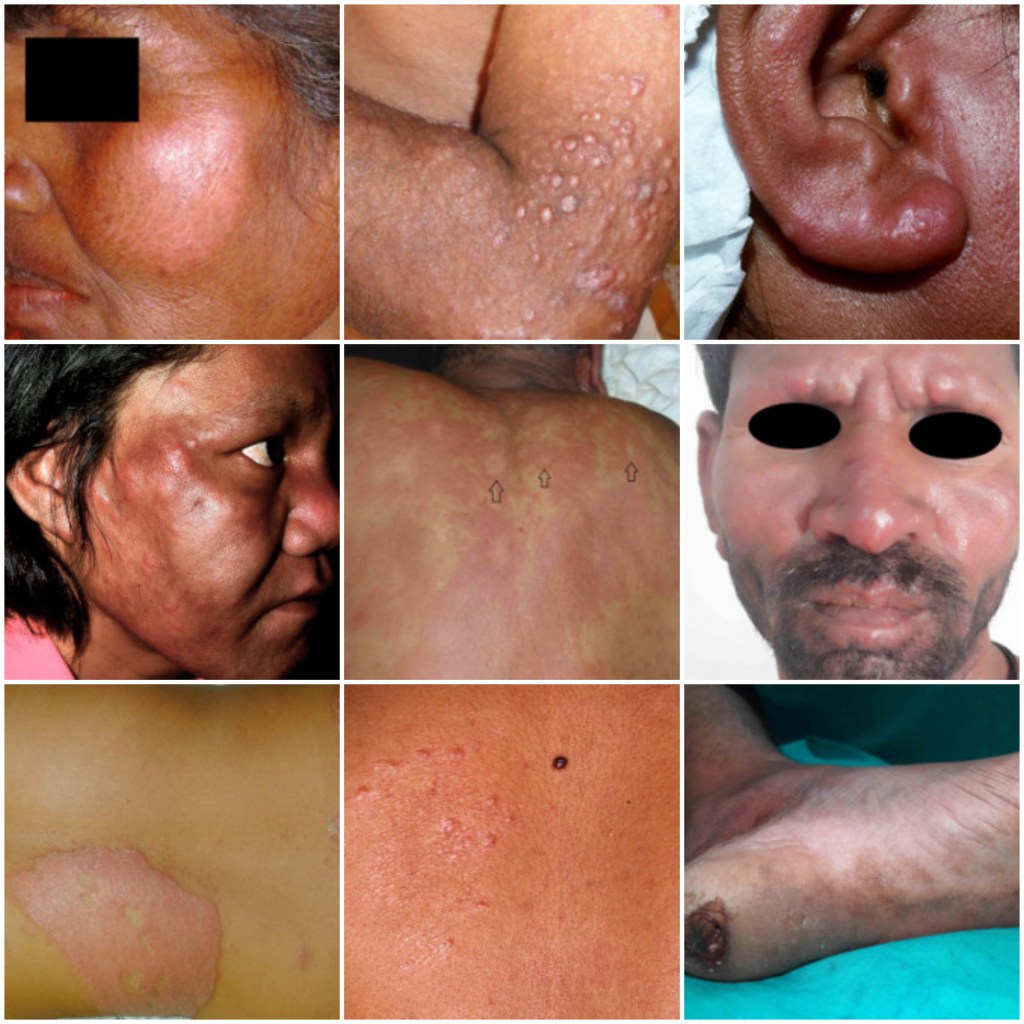
Images from DermNet NZ
Complications
Since leprosy often causes loss of sensation, it is likely that an affected individual may not feel injuries such as cuts and burns, thereby making them more vulnerable to serious damage to affected parts of the body. In some cases, damage could be so severe that amputation of digits or limbs may be required.
In addition, if the infection remains undiagnosed and/or untreated, there is a possibility of experiencing one or more of the following complications:
- shortening of digits (fingers and/or toes) as they get reabsorbed by the body
- paralysis of hands and/or feet
- nose disfigurement
- blindness
- chronic ulcers on soles of feet
- risk of secondary infections where skin is dry and damaged
It is this occasional shortening of digits and amputation of limbs that, in early years, had given rise to the mythical ideology that leprosy causes “limbs to fall off”.
Causes
Leprosy is caused by a slow-growing bacterium known as Mycobacterium leprae. Infection is believed to occur by means of droplet transmission, where one inhales or ingests contaminated droplets that have been coughed or sneezed out by an infected person. In most cases, it seems that newly infected individuals were in prolonged, close contact with an untreated leprosy patient prior to their own infection.
In certain parts of the world such as the southern United States, infection is also said to occur through armadillos who are believed to be naturally infected with M. leprae.
Diagnosis
Being slow-growing in nature, M. leprae has an incubation period that may last from between six months to 20 years. On average, symptoms are observed about five years after infection.
The most obvious means of diagnosis is the observation and identification of some or all of the symptoms mentioned above.
A skin smear test would usually be carried out, where smear samples (usually from several affected areas on the skin) would be taken to test for acid-fast bacteria, a characteristic of M. leprae. A negative test at all sites indicates that the condition is paucibacillary (PB) leprosy, implying that there is no evidence of more advanced disease. A skin or nerve biopsy would confirm this. A positive test at any site indicates multibacillary (MB) leprosy, reaffirming the presence of M. leprae and implying the presence of advanced disease. Again, a biopsy would confirm this.
[Note: Until a few years ago, a more complex categorisation of leprosy was used on the basis of microscopic patterns observed. These were intermediate (I), tuberculoid-tuberculoid (TT), borderline tuberculoid (BT), borderline-borderline (BB), borderline lepromatous (BL) and lepromatous-lepromatous (LL). The WHO later simplified the diagnostic classification to PB leprosy (equivalent to I, BT, BT) and MB leprosy (equivalent to BB, BT and LL).]
Prevention
Despite the potential severity of the disease, there is still no vaccine available against leprosy. In some parts of the world, the BCG (Bacillus Calmette Guerin) vaccine used against tuberculosis is administered in the hope that it would double as a preventive agent against leprosy as well. This is based on the fact that the two types of bacteria that cause tuberculosis (Mycobacterium tuberculosis) and leprosy (Mycobacterium leprae) are somewhat closely related. However, while this may have some sort of impact on a recipient’s reaction on exposure, there are no data or statistics to confirm that this is indeed an effective method to prevent M. leprae infection.
Hence, the most effective way to prevent further transmission of the disease is to facilitate an early diagnosis (i.e., having a medical examination done as soon as symptoms are noticed), as well as to compliantly complete the entire course of medication prescribed by your doctor upon diagnosis.
In cases where exposure to an infected person is known or suspected, rifampicin may be administered to reduce the chance of developing PB leprosy.
Treatment
A multi-drug therapy (MDT) approach is used in the treatment of leprosy as previous use of a single antibiotic has shown to result in antibiotic resistance (https://thebiolog.com/2020/02/11/antibiotic-resistance/) in M. leprae. The most commonly used combination includes dapsone, rifampicin and clofazimine, prescribed for six months in the case of PB leprosy and twelve months for MB leprosy. The doctor handling a given case would prescribe medication according to each individual’s case, and would also recommend tests to be carried out periodically in order to monitor the progress of the recovery.
If taken compliantly in a timely diagnosis, this line of treatment can completely cure a patient of leprosy. However, in cases of a late diagnosis or commencement of treatment after the disease has advanced, a patient may be left with permanent disability or disfiguration pertaining to their specific case, even after they have been cured of the infection. (Patients are generally thought to be non-infectious once treatment has begun. Yet, it is always best to take relevant precautions in order to prevent the spread of disease.)

Image from WeCapable
Cover illustration adapted from Depositphotos.
