Dental caries – cavities or tooth decays, as they are commonly known – are caused by harmful bacteria in our mouth that feed on sugar and starch in food we consume, and produce acids as a by-product. Over time, these acids could attack and damage the teeth, starting with the enamel and working their way further inside if not dealt with. The image below shows a simple illustration of this phenomenon.
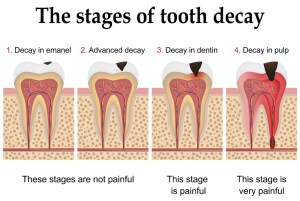
With each round of acid production, there is some mineral loss that occurs in our teeth. However, this is regained from calcium and phosphate minerals present in our saliva and from external sources such as fluoride in toothpaste, and other foods that boost oral health. This is a natural process that takes place on a daily basis.
Brushing our teeth, flossing and rinsing our mouth are mechanisms that can help to remove some of the acid produced, food particles and plaque (a thin film of bacteria on our teeth) from our teeth. However, frequent consumption of sugar- or starch-rich food and beverages and insufficient or improper oral hygiene practices could off-set the mineral loss-mineral gain balance, causing a mineral deficiency in teeth. Initially, these appear as white spots, which are the preliminary sign of tooth decay. At this point, the damage may be reversible, if detected in time and countered with fluoride toothpaste and other mineral sources, together with our own saliva.
If the decay is allowed to continue, it progresses to the next stage where further mineral loss damages and weakens the outer enamel. If still left untreated, decay could reach the inner dentin layer, and eventually the softer pulp within and below the tooth. This could lead to more serious infections and a quite a bit of pain.
Symptoms
The symptoms of tooth decay are usually straight forward and include:
- spontaneous, intermittent or continuous toothache
- sensitivity to sweet, hot or cold food or drink
- pain when biting into or chewing food
- black, brown or white discolouration of teeth
- pits or holes in teeth
Complications
If left untreated, tooth caries may worsen and lead to complications that include:
- severe pain that interferes with daily functioning
- tooth abscess with pus formation and inflammation in the surrounding or underlying gum
- damaged or broken teeth
- shifting of teeth (widened gaps) over time due to tooth loss
- confidence issues due to visible loss of or discoloured teeth
- problems eating or drinking, leading to nutritional deficiencies in extreme cases
- nerve infection or septicaemia as a result of abscesses, in rare and extreme cases
Causes
While the cause of dental caries is straightforward, as outlined above, there are certain factors that increase the risk of its incidence. These include:
- location of teeth, with those at the back being more prone to decay due to the presence of more grooves and pits, as well as being less accessible for brushing and cleaning in comparison to front teeth
- not brushing teeth frequently, or not rinsing after eating or drinking anything other than water
- inadequate fluoride exposure
- frequent consumption of sugary or acidic food and beverages
- dry mouth arising from reduced saliva production caused by certain medications, treatments or medical conditions
- age – young children and older adults have been found to be more prone to dental caries
- feeding infants before bedtime, as beverages such as milk, juices, formula, etc. cling onto their teeth for hours while they sleep
- worn out fillings or ill-fitting dental devices
- GERD, which could cause a reflux of acid into the mouth
- eating disorders such as anorexia and bulimia, where repeated vomiting could result in teeth being repeatedly exposed to stomach acids, and also could interfere with saliva production
Diagnosis
If any of the symptoms mentioned above are observed, a visit to your dentist would enable them to give a clear diagnosis and advice on your condition.
Prevention
Here are a few measures that we can take in order to prevent the incidence of tooth decay:
- brush your teeth at least twice a day
- use a toothpaste (and mouth-wash, if you use one) that contains fluoride
- floss regularly – at least once a day
- rinse your mouth after eating
- visit your dentist at least once a year for a clean-up and to check on your overall oral health
- do not eat or drink anything other than water after brushing your teeth at night
- avoid regular consumption of sugary or acidic foods, and frequent snacking and sipping of beverages other than water
- speak to your dentist about getting a protective layer of dental sealant on your teeth (particularly hind teeth) if your teeth seem prone to decay – this usually lasts a few years before needing replacement
- include foods that are good for oral health in your diet – such as calcium-rich foods (dairy, almonds, soy, tofu, salmon, green leafy vegetables), phosphorous-rich foods (eggs, dairy, nuts, fish, white meat, beans), vitamin C-rich foods for gums (citrus fruits, pepper, tomato broccoli, spinach)
Treatment
If initial decay – or rather the precedent white spotting – is detected, the ideal thing to do would be to increase the amount of minerals that the tooth or teeth are exposed to, to help their rebuilding process. As mentioned before, this would be in the form of fluoride toothpaste (and even mouthwash), and mineral rich food and beverages such as mentioned above.
For decay that has progressed beyond this stage, one of the following may be advised by your dentist, depending on the progress of the cavity:
- filling, where the decayed part of the tooth is restored with a suitable material such as porcelain, composite resins, metal or dental amalgam. This is usually the most common treatment form for decay that has progressed just beyond the initial stage.
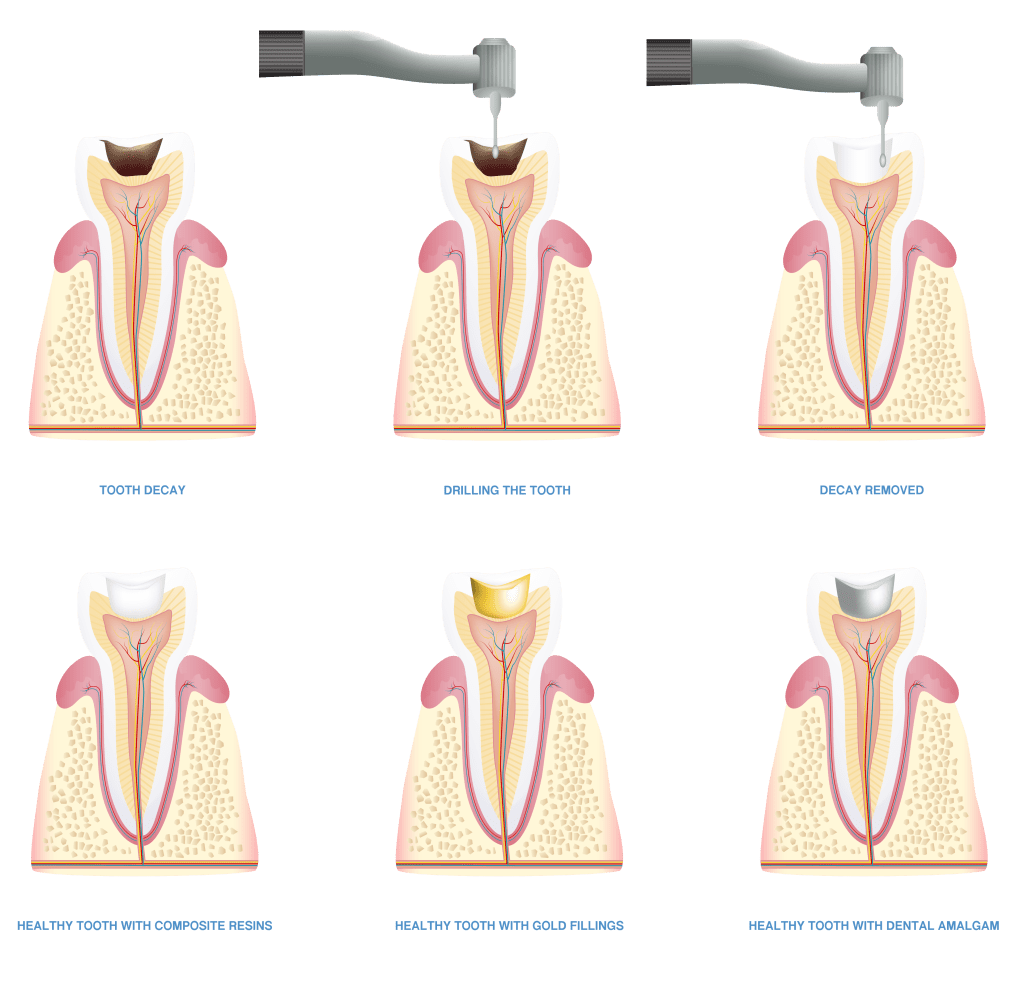
Image from Willow Pass Dental Care
- crown, where a custom-made covering is fitted onto the top of the tooth to replace its original crown. This is usually done where decay has progressed to a point where the tooth is significantly damaged or weakened. The dentist usually drills out the entire damaged part of the tooth prior to fixing the crown. Porcelain, resin, metal, or a combination may be used.
- root canal, where the pulp is replaced with a filling. This is usually administered where decay has reached the pulp, often causing infection inside, and is the last option available to try to save the damaged tooth. This procedure should be done with care by a known and trusted professional.
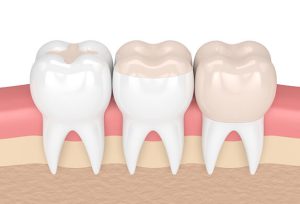
Image from Smiles Dental
- extraction, where the tooth is removed as it has progressed beyond the stage of redemption. This may later be followed by a dental implant or the use of a bridge to close the resulting gap and prevent the shifting of teeth. However, care must be taken if a bridge is used as there is a possibility of neighbouring teeth getting damaged.
Cover Illustration adapted from Illustoon.
